Muscle strains (pulled muscles) are common but painful injuries. You can often treat a pulled muscle at home. But not all strains are alike: A severe tear might need medical care or even surgery. Follow your healthcare provider’s advice to ensure a smooth recovery.
What Is a Muscle Strain?
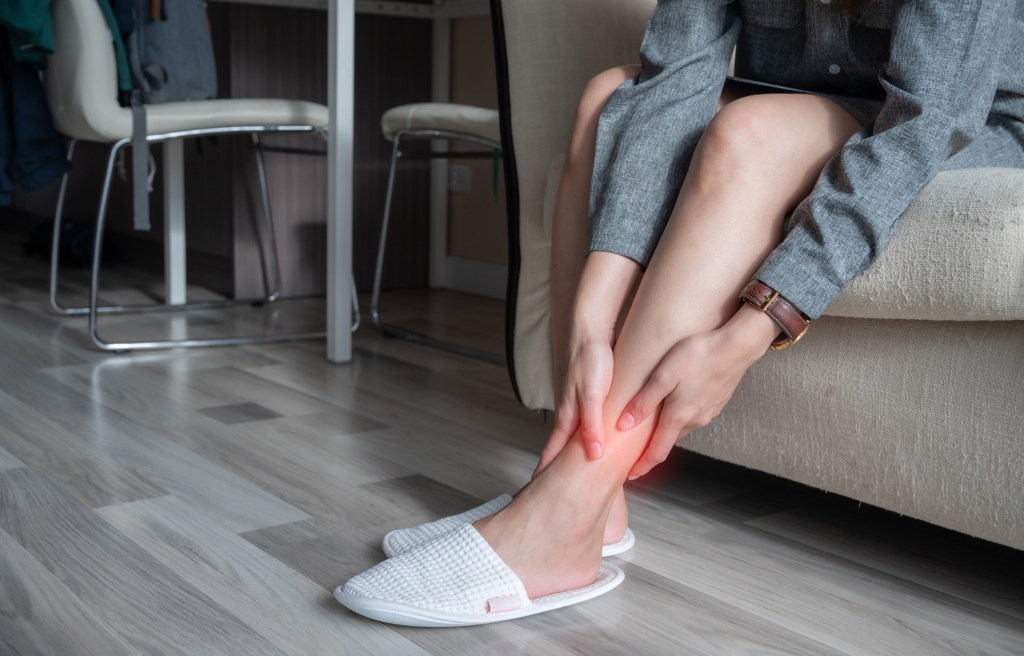
A muscle strain, or pulled muscle, is a tear in your muscle fibers. It’s one of the most common soft tissue injuries. You can strain a muscle by pulling it too hard or using it too much, which weakens the fibers.
Muscle strains can be minor to major. A mild strain might only break tiny fibers within the fabric of your muscle, while a severe one can tear through it. Strains are painful, but most can heal with time and rest.
Your muscles are made of thousands of small fibers woven together. When you strain a muscle, the strands of fiber are stretched beyond their limit and tear apart. If you’ve ever tried to use an old bungee cord to hold something in place, you’ve seen this happen. New bungee cords have plenty of give and stretch. But if you use one for too long or suddenly jerk on it too hard, the fibers will start to pull apart.
Types of muscle strains
Common types of muscle strains include:
- Abdominal muscle strain
- Back strain
- Groin muscle strain
- Hip flexor strain
- Calf muscle strain
- Hamstring strain
Healthcare providers also classify muscle strains as either acute or chronic.
- Acute muscle strains. These happen suddenly and cause immediate symptoms. You might pull a muscle with a sudden, forceful movement, or by twisting it.
- Chronic muscle strains. These develop gradually, and so do the symptoms. You can gradually tear a muscle by overusing it without giving it enough time to repair.
Muscle tears symptoms
Symptoms of a pulled or torn muscle include:
- Muscle pain
- Muscle spasms
- Bruising
- Swelling
- Muscle weakness
- Limited range of motion
- Feeling a “pop” during the injury
- Seeing a gap or dent in the shape of the muscle
What does a torn muscle feel like?
A torn muscle feels sore when you try to use it. You can usually locate the pain in one spot. You may be able to connect it to a recent event or activity. If it’s a chronic muscle strain, you may develop pain gradually over a few days. If it’s an acute muscle strain, you’ll feel pain immediately, and it may even feel like tearing. You may also feel your muscle weaken, and you may feel that you can’t use it at all.
Causes of muscle strains
Muscle strains happen when you tear the fibers of your muscle. This can happen suddenly or gradually.
Common causes of muscle strains include:
- Acute injuries. Muscle strains are often sports injuries, caused by sudden sprinting, twisting or jumping. But accidental muscle strains are also common in everyday life.
- Repetitive strain injuries. Repeating the same movement over and over, whether at work or a recreational activity, can strain your muscles over time.
- Overtraining. Training or laboring too hard or too long without letting your muscles rest weakens them. If they don’t have a chance to rebuild, they might break instead.
- Undertraining. Low flexibility and strength can cause muscles to strain with ordinary use. Not stretching or warming up before exercise can overstress your muscles before they’re ready.
Risk factors of muscle strains
Some muscles are more likely to tear than others. These are muscles that:
- Cross more than one joint. Muscles that cross joints often act to restrain other muscles when you move that joint. If the joint moves with too much force, these muscles feel the impact first.
- Contract eccentrically. Eccentric muscles stretch and lengthen when bearing a load. They absorb the impact of the load with controlled movements, like lowering a weight or walking downhill.
- Have type II muscle fibers. Muscles with higher concentrations of type II muscle fibers (fast-twitch fibers) are designed for short bursts of power and speed, so they use more force.
Other risk factors that can contribute to muscle strains include:
- Muscle stiffness. When muscles are tight and inflexible, the fibers break more easily.
- Muscle imbalances. Favoring some muscles over others can make the others too weak.
- Previous injuries. Muscles that have been torn before are more likely to tear again.
How is a muscle strain diagnosed?
If you’ve pulled a muscle, you’ll probably have a pretty good idea of how it happened. A healthcare provider will start by asking you about when the pain started and what you were doing at the time. Then, they’ll examine the spot, which may have visible bruising and swelling if it’s been at least 24 hours since the injury. They’ll gently feel it for tenderness and test the muscle for strength and range of motion.
A physical exam is often enough to diagnose a pulled muscle. But in some cases, your provider might want to take an MRI to rule out other conditions, or to determine the extent of the tear and grade it.
Muscle strain grades
Healthcare providers also grade muscle strains by how severe they are.
- Grade I. If you have a mild muscle strain, you’ve stretched and pulled your muscle enough to cause minor damage, but it isn’t torn through. This is the most common type.
- Grade II. A moderate muscle strain has torn through some or even most of the muscle. This will affect your muscle strength and range of motion. It can take time to heal.
- Grade III. If you have a severe muscle strain, your muscle has torn all the way through. A complete muscle tear (muscle rupture) might need surgery to repair it.
What’s the best treatment for a pulled muscle?
Most people can recover from a pulled muscle at home. Only a severe, grade III tear might need surgery. Surgery for a complete muscle tear means stitching the two ends of the muscle back together.
Home treatment for a muscle strain includes:
- The RICE method. Rest, ice, compression and elevation can help relieve pain and inflammation during the first few days of your recovery. After the first few days, you can start moving it again.
- Crutches. If your injury is in your lower body, you might need to use crutches to keep weight off the muscle when you walk. Your healthcare provider can guide you on how long to use them.
- Pain relievers. Anti-inflammatory medications, like NSAIDs, can help during the first few days of your recovery. After this, your healthcare provider might recommend switching medications.
- Physical therapy. It’s important to reintroduce gentle movement after the first few days of recovery. A physical therapist can guide you in specific exercises to rehabilitate your muscle.
- Platelet-rich plasma injections. This newer treatment uses platelets from your own blood to stimulate tissue repair. It’s still unproven, but some studies suggest it can speed up healing.
When should I see a healthcare provider for a muscle strain?
Check in with a healthcare provider if your muscle strain:
- Seems severe. If you heard or felt a “pop” when your muscle tore, if you can’t move your muscle at all, or if pain, bruising and swelling are severe, see a provider right away.
- Isn’t improving. If symptoms persist or get worse after a few days, your injury might not be as minor as you thought. It’s time to have a provider examine it.
- Triggers new symptoms. If you develop nerve-related symptoms like numbness, tingling, sudden weakness or difficulty controlling certain muscles, you may have nerve damage.
You might want to ask:
- Which muscle did I strain?
- What grade is my muscle strain (how bad is it?)
- What activities should I avoid during recovery?
- How long should I rest, and when should I start moving again?
How long does a pulled muscle take to heal?
If you only have a minor (grade I) muscle strain, it should heal within a few weeks. Moderate (grade II) muscle strains may take several weeks to months to heal completely. A severe (grade III) muscle strain can take four to six months to heal after surgery. You may need to immobilize your muscle with a cast for up to six weeks before starting your rehabilitation program. Athletes will need to sit out the season.
Most people recover completely from a muscle strain, even a severe one. But how you treat your muscle during recovery can affect how well it heals. In some cases, the muscle might retain some scar tissue, which is stiffer and more brittle than healthy muscle tissue. This makes it easier to tear the muscle again. You might have to be more mindful of how you use your muscle in the future.
What can I do to prevent muscle strains?
Some simple guidelines to help prevent muscle strains are:
- Condition your muscles with a daily fitness program.
- Stretch and warm up your muscles before using them.
- Check your technique when lifting weights or performing physical tasks.
- Pay attention to your posture and workplace ergonomics.
A note from QBan Health Care Services
Pulling a muscle is painful. For some, the frustration of having to sit out of your favorite sports and activities while you recover can be just as difficult. But your muscle needs time to heal, and it needs your patient attention during the rehabilitation process. Giving yourself that time is the best way to ensure you’ll be able to return safely to doing what you love to do, at the intensity level you’re used to.