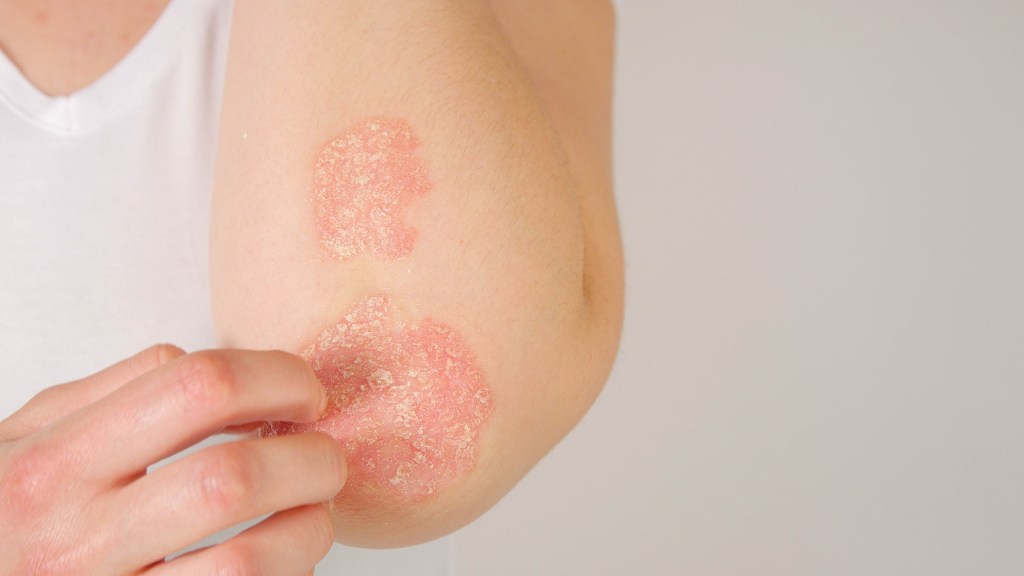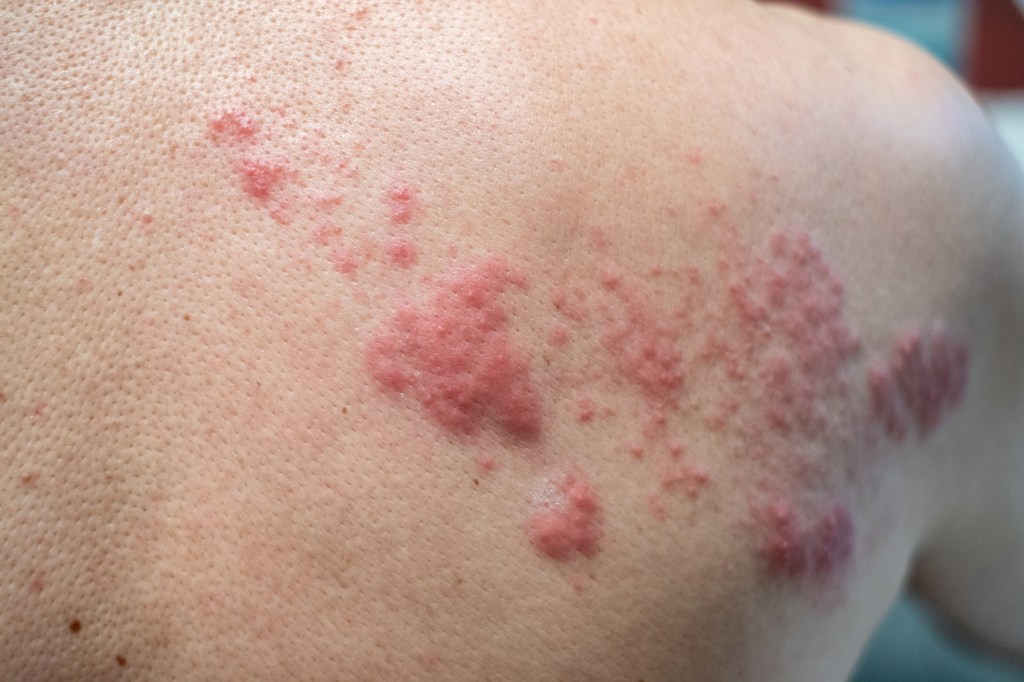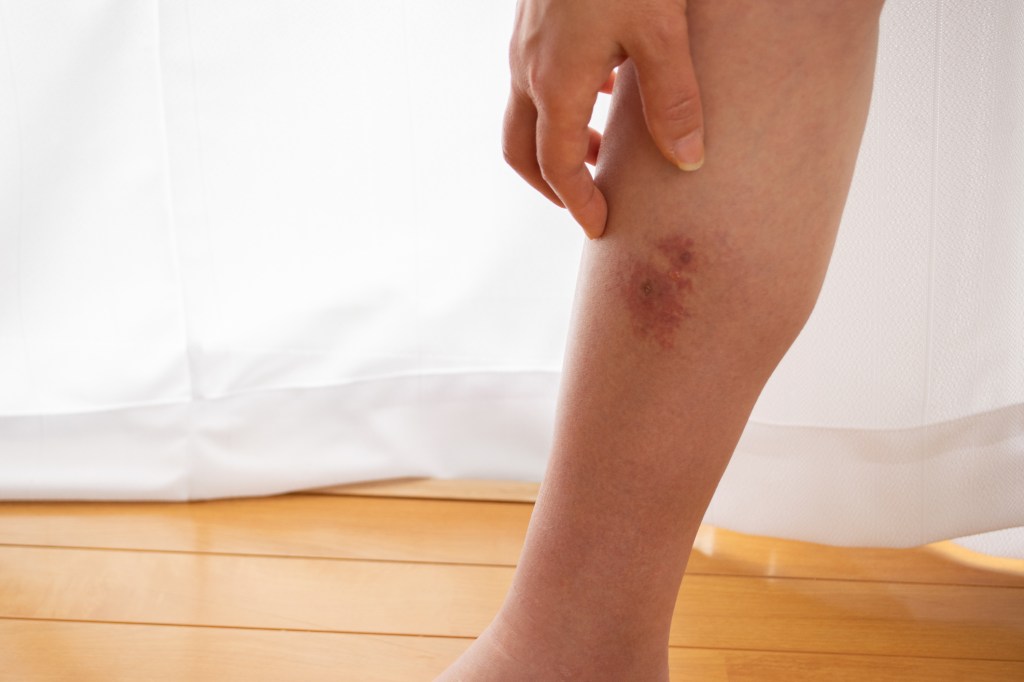
Cellulitis is a bacterial infection of your skin and the tissue beneath your skin. Anyone can get cellulitis, but the risk is higher if you have a skin wound that allows bacteria to enter your body easily or a weakened immune system. Treatment includes antibiotics. A warm compress, elevation, compression and NSAIDs also help relieve your symptoms.
What is cellulitis?
Cellulitis is a bacterial infection of your skin and the tissues beneath your skin. It most commonly affects the lower part of your body, including your legs, feet and toes. However, it can occur in any part of your body. It also commonly appears on your face, arms, hands and fingers.
Who does cellulitis affect?
Anyone can get cellulitis. However, you may be more likely to get cellulitis if:
- You’re a child.
- You have a wound such as a cut, ulcer, bug bite, animal bite, surgical incision, tattoo or piercing.
- You have a long-lasting (chronic) skin condition such as athlete’s foot, eczema or psoriasis.
- You have chickenpox or shingles.
- You have a weakened immune system.
- You have obesity.
How common is cellulitis?
Cellulitis is very common. There are more than 14 million cases of cellulitis in the United States per year.
How does cellulitis affect my body?
Cellulitis causes swelling and pain. If you have cellulitis on your hands or feet, it may be challenging to close your hands or walk.
A cellulitis infection may cause flu-like symptoms, including a fever higher than 100 degrees Fahrenheit (38 degrees Celsius), chills, sweats, body aches and fatigue.
What are the symptoms of cellulitis?
Symptoms of cellulitis may include:
- Pain.
- Tenderness.
- Edema (swelling).
- Warmth.
- Discoloration (red, purple or slightly darker than your usual skin color) that may look like a rash.
- Fluid-filled blisters.
- Skin surface looks lumpy or pitted, like an orange skin.
- Fever.
- Chills.
- Fatigue.
What is the main cause of cellulitis?
Many different bacteria can cause cellulitis. However, Streptococcus (strep) and Staphylococcus (staph) cause most cases of cellulitis.
Is cellulitis caused by poor hygiene?
Cellulitis usually appears around damaged skin, but it also occurs in areas of your skin with poor hygiene.
You can maintain good skin hygiene by:
- Washing your hands regularly with soap and warm water.
- Cleaning and trimming your fingernails and toenails.
- Regularly showering and thoroughly drying your skin after.
- Wearing clean clothes.
- Keeping small wounds clean.
What does the beginning of cellulitis look like?
When you first get cellulitis, your skin looks slightly discolored. It may feel slightly warm to the touch. As the infection spreads, the discoloration gets darker as your skin swells and becomes tender.
Is cellulitis contagious?
Cellulitis isn’t usually contagious. Though rare, you may be able to contract cellulitis if you have an open wound and have skin-to-skin contact with an infected person’s open wound.
How is cellulitis diagnosed?
To diagnose cellulitis, your healthcare provider will ask about your symptoms and perform a physical examination of the affected area.
What tests will be done to diagnose cellulitis?
In most cases, your healthcare provider won’t conduct any tests. However, if you’ve got a severe case of cellulitis, your healthcare provider may recommend tests to make sure the infection hasn’t spread to other parts of your body.
These tests may include:
- Blood test. A blood test will confirm whether the cellulitis infection has spread to your blood.
- Skin test. A skin test will identify the type of bacteria responsible for your cellulitis, which helps your healthcare provider prescribe the most appropriate antibiotic.
- Bacterial culture. A bacterial culture will identify the type of bacteria responsible for your cellulitis.
How is cellulitis treated?
Your healthcare provider will typically prescribe antibiotics taken by mouth (oral antibiotics) to treat your cellulitis. Oral antibiotics may include dicloxacillin or cephalexin.
Severe cases of cellulitis may not respond to oral antibiotics. You may require hospitalization and intravenous (IV) antibiotics — your healthcare provider will use a small needle and tube to deliver the antibiotics directly into a vein.
What is the fastest way to get rid of cellulitis?
The fastest way to get rid of cellulitis is to take your full course of antibiotics. Some home treatments may help speed up the healing process.
Home treatments include:
- Warm compress. Apply a warm compress to your affected area to help reduce swelling and other symptoms.
- Elevation. Elevating your affected area helps lower the blood pressure in the area’s blood vessels and improve blood flow.
- Compression. Compression wraps or stockings help reduce swelling and improve blood flow. Don’t wrap your affected area too tightly. This can cut off circulation. Remove the compression wrap or stocking at least twice every day for 10 to 15 minutes.
- Non-steroidal anti-inflammatory drugs (NSAIDs). Over-the-counter (OTC) NSAIDs, such as aspirin, ibuprofen and naproxen, reduce pain and inflammation. Not everyone can take NSAIDs, so it’s a good idea to check with your healthcare provider before use.
How soon after treatment will I feel better?
In most cases, you should feel better within seven to 10 days after you start taking antibiotics.
You’ll notice signs that your cellulitis infection is healing a few days after starting antibiotics. Your pain will decrease, swelling will go down and any discoloration will begin to fade.
How can I reduce my risk?
You can reduce your risk of developing cellulitis by:
- Cleaning your wounds or sores with antibacterial soap and water.
- Applying an antibiotic ointment on your wounds or sores.
- Covering your wounds or sores with a bandage to prevent dirt or bacteria from entering the area.
- Refraining from touching or rubbing your affected areas.
- Getting medical attention right away for any deep cuts or puncture wounds.
What can I expect if I have cellulitis?
With early diagnosis and treatment, the outlook for people with cellulitis is good. Most people feel better after seven to 10 days.
It’s very important to take cellulitis seriously and get treatment right away. Cellulitis can quickly progress and lead to more severe conditions. The bacteria could spread to your bloodstream (bacteremia) or heart (endocarditis), which may be fatal.
How do I take care of myself?
- Follow your healthcare provider’s instructions. It’s important to finish your full course of antibiotics, even if you start to feel better. If you don’t finish your full course of medicine, your cellulitis may come back and be more challenging to treat.
- Refrain from touching the affected area. If you must touch the affected area, wash your hands before and after touching it. Don’t squeeze or puncture the area. Squeezing and puncturing won’t drain any swelling or provide relief.
- Rest. It’s a good idea to avoid any activities that may aggravate your affected areas, including walking, running or other exercises.
When should I see my healthcare provider?
Call your healthcare provider if:
- You notice an increase in swelling, discoloration or pain.
- Your symptoms don’t go away a few days after starting antibiotics.
- Your cellulitis infection spreads to surrounding areas of your body.
What questions should I ask my healthcare provider?
- How do you know that I have cellulitis?
- If I don’t have cellulitis, what other condition might I have?
- How did I get cellulitis?
- What bacteria caused my cellulitis?
- For how long and at what times of the day should I take my medication?
- How should I store my medication?
- When will I start to feel better?
- Do I need to schedule a follow-up visit?
- What activities should I avoid?
- Which OTC pain relievers do you recommend?
Does cellulitis itch?
No, cellulitis doesn’t itch. However, your affected area may itch once your skin starts to heal.
Why do I keep getting cellulitis?
Many people who get cellulitis again usually have skin conditions that don’t go away without treatment, such as athlete’s foot or impetigo. Poorly controlled diabetes may also contribute to repeat instances of cellulitis.
Approximately 33% of all people who have cellulitis get it again.
A note from QBan Health Care Services
Cellulitis is a common skin condition that mostly affects children and people with wounds, chronic skin conditions or a weakened immune system. If you notice symptoms of cellulitis, talk to your healthcare provider right away. They’ll prescribe you an antibiotic to quickly clear up the bacterial infection and recommend home treatments to make you more comfortable.
To prevent cellulitis, be sure to practice proper hygiene. Clean any wounds with water and antibacterial soap and cover them with a clean bandage to reduce your risk of infection.